What to expect in ICU
An outline of what to expect when in ICU and after transfer to the ward.
Admission to ICU
You may be admitted from ICU from a number of areas, such as:
- From the Emergency Department if you are too unwell to be admitted onto a ward
- From a ward if your health has deteriorated and you need closer monitoring and management
- Directly transferred from one hospital to the Alfred ICU. This may be if your health is very complex and requires the skills and services only available at the Alfred ICU
- Directly from the operating theatre or procedure room. This may be planned in advance if you are having complex surgery which requires intensive care for a period afterwards, of if you are unwell in the post-operative period and require closer monitoring
The Alfred has intensive care beds on level one and level three. Both ICUs offer a high standard of specialist care and the ICU you are admitted to does not indicate the level of care you require.
ICU Patient Care
For information on common treatments and therapies that are provided in the ICU please view the following document.
Length of stay in ICU
The length of time a patient spends in ICU depends on how ill they are and may vary from a few hours to a number of months, although for the majority of patients, it is usually less than one week.
Depending on how sick you are, you may have your own nurse, or a nurse shared between two patients.
After ICU
When you are well enough to require less intensive monitoring and management, you are transferred to a ward.
This is a positive step and usually a sign that your health is improving. Patients and families may feel anxious about the prospect of leaving the ICU, especially if your stay with us has been a long one. You may have developed close relationships with the nurses and doctors in the ICU, the technology and constant monitoring may have made you feel secure.
Our ward staff are familiar with caring for patients who have been in the ICU and will continue the care required.
Our Patient Access Nurses liaise with the wards to co-ordinate discharges and a smooth transfer from the ICU to the ward.
On the ward
On the ward, nurses will be caring for other patients as well. You will be able to call for the nurse at any time by using the call bell. As part of patient care plans the staff will encourage independence.
As strength and condition improves, patients usually need less assistance and intervention from staff.
ICU Involvement on the ward
ICU involvement in patient care continues after transfer to the ward.
The Intensive Care Outreach Service will visit you once discharged and monitor your progress on the wards. The Intensive Care Outreach team is made up of both medical and nursing staff who visit patients on the ward within 24 hours of discharge from ICU. The team will assess progress and ensure plans put in place on transfer from the ICU continue on the ward.
We endeavour to lessen patient and family anxiety by preparing you early for the transfer to the ward and by maintaining contact with our follow up visits. Patients are reviewed as often as necessary by our Intensive Care Outreach Service.
Recovery
Recovery is different for all patients. Some patients spend only a short period in the ICU whereas others may spend weeks or months. Some patients will be much sicker than others. It is sometimes difficult to predict the rate of recovery and outcome as all patients are different. The following are some general issues that patients may experience after leaving the ICU.
General weakness – As patients recover, it may become apparent just how weak they are. Sitting out in a chair may be exhausting at first. The nurses and physiotherapists will help patients to regain their strength and set realistic goals for recovery. In the beginning, short term achievable goals are recommended. Plenty of rest between activities will help regain some strength.
Sleep deprivation –The ICU environment is often not good for sleep and it is easy to lose day-night routine. The ward is generally quieter and patients require fewer interventions. In this environment sleep patterns will return to a more natural state. Some patients have described experiencing bad dreams or nightmares following their ICU stay. These usually subside over time but patients may find it helpful to talk to family, friends or the nurse if these occur.
Amnesia/delusions – Some patients may not remember what happened to them whilst in the ICU. Patients might also think they remember something that didn’t happen at all. If patients would like more information about their stay in the ICU or would like to talk to someone about these issues ask to see the ICU Liaison Nurse.
Eating and drinking well – Depending on the patient’s circumstances, it may take some time before they can eat and drink well enough to maintain nutritional requirements. A dietitian will monitor nutritional status and food will be provided either to eat normally or via a feeding tube.
When patients do start to take food and drink orally they may notice it tastes different or the mouth may be sore. This should resolve fairly quickly but let the nurse know of any concerns.
Digestive alterations – Patients may experience constipation, diarrhoea, bloating, or stomach ache as they recover. These symptoms may be the result of serious illness, surgery or drugs. Make sure you let the nurse know if your loved one is experiencing any of these symptoms so a treatment plan can be developed.
Leaving hospital
Another big step in recovery is when you are well enough to leave hospital. Both patient and loved ones may feel apprehensive and also excited about the next step. Preparation for discharge will involve meeting with a variety of health professionals in the ward, such as social workers, occupational therapists and rehabilitative consultants.
Discharge destination may be home or a rehabilitation facility depending on individual needs.
Once discharged from hospital, you may realise the full impact of your hospital stay, the critical illness and subsequent decrease in general ability. Physical difficulties such as muscle weakness, joint stiffness, numbness, sleep and taste disturbance, hair loss and skin changes become more apparent at home. Some patients have said even when they are at home they continue to have dreams and flashbacks about their ICU experience.
We suggest setting short-term, achievable goals. Don’t try to overcome all problems at once. There are help and support groups in the community. The social work department will be able to help identify supports available to you.
You will generally need to return to the hospital for outpatient appointments. Outpatient appointments are with your treating medical staff or sometimes with the allied health departments depending on individual needs. Appointments are arranged on the day of discharge.
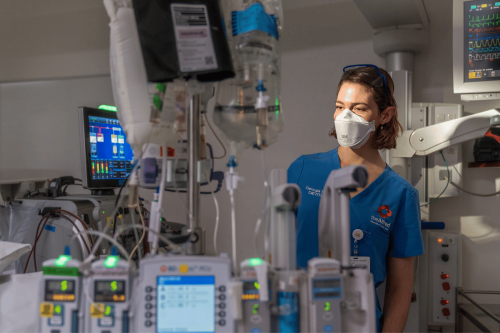
About our Intensive Care Unit (ICU)
The Intensive Care Unit (ICU) at The Alfred is a specially staffed and equipped unit that provides care for patients with life threatening or potentially life threatening conditions.
Find out more
Visiting the ICU
There are a number of conditions when visiting ICU, including who can visit, when and how to make a booking.
Read more