Late effects: Lung health
The lungs are very important organs that supply oxygen to the body. Sometimes, treatments for blood disorders can cause lung damage. If you received any treatments that may cause lung problems, it is important to learn about the lungs, and what you can do to keep them as healthy as possible.
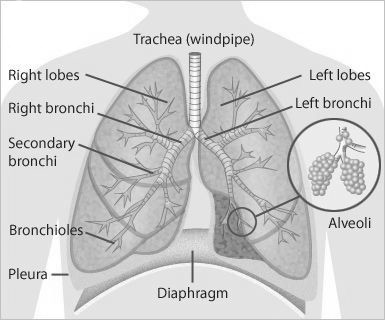
How do the lungs work?
The lungs transfer oxygen from the air to the blood, where it is circulated to the body tissues. The lungs also remove carbon dioxide, a waste product made by the body’s cells.
In order for oxygen to reach the blood, it must move through tiny air sacs (alveoli) in the lungs and into tiny blood vessels (capillaries) that surround each air sac. When the air sacs become damaged or scarred, there is less area for oxygen to enter the bloodstream and less oxygen reaches the blood. You may then need to breathe faster in order to get enough oxygen. This can make you feel short of breath.
Other lung problems can be caused by inflammation (swelling) of the air passages in the lungs or increased mucous production as a result of irritation or infection. Symptoms can include cough, wheezing, chest pain, and shortness of breath.
Am I at risk of lung problems?
If you received any of the following treatments during your cancer therapy, you may be at risk for developing lung problems:
- Bleomycin
- Carmustine (also known as BCNU)
- Lomustine (also known as CCNU)
- Busulfan
- Radiotherapy to the chest
- Surgery to the chest or lung (this does not include surgery for placement of a central line, such as a Hickman)
- Stem cell transplant from a donor other than yourself (allogeneic transplant), if you then developed chronic graft versus host disease (chronic GVHD)
- Certain chemotherapy drugs known as anthracyclines, such as daunorubicin, doxorubicin and idarubicin can damage the heart and may contribute to lung problems, especially if given in combination with bleomycin, BCNU, CCNU, and radiation treatment
Other factors that may increase your risk are:
- Younger age at the time of cancer treatment
- A history of lung infections, asthma or other lung problems
- Tobacco use, marijuana use or exposure to second hand smoke
- Graft versus host disease of the lungs
What problems can develop?
Problems can include scarring of the lungs (pulmonary fibrosis), repeated lung infections (such as chronic bronchitis, bronchiectasis, or recurrent pneumonia), inflammation of the lung tissues and small airways within the lungs (bronchiolitis obliterans), and rupture of the tiny air sacs in the lungs or thickening and blockage of air passages within the lungs (restrictive/obstructive lung disease).
What are the symptoms of lung damage?
Symptoms may include shortness of breath, frequent coughing and/or wheezing, chest pain, and frequent lung infections, such as bronchitis or pneumonia.
Becoming easily fatigued or short of breath during mild exercise (exercise intolerance) is sometimes an early symptom of lung damage.
What monitoring is recommended?
A yearly medical check-up is recommended.
A chest x-ray and pulmonary function tests may show lung problems that are not apparent during a check-up. For this reason, it is helpful to have these tests done at least once (at least two years after completing cancer treatment) to find out if there are any problems. Your doctor can decide if further testing is needed based on these results
Are there any special precautions I should take?
If you have had any of the treatments listed above you should:
- Get the pneumococcal (pneumonia) vaccine
- Get yearly influenza (flu) vaccines
- Avoid SCUBA diving, unless you have undergone a thorough medical evaluation and received clearance from a diving medicine specialist
What can I do to prevent lung problems?
You can prevent lung problems if you:
- Don’t smoke. If you do smoke, then quit. Quitting is the most important thing you can do to keep your lungs and you healthy
- Avoid second-hand smoke
- Get regular physical exercise
- Avoid breathing toxic fumes from chemicals, solvents, and paints
Where can a smoker find help to quit?
Your most important resources for quitting smoking are your family, friends and your doctor. You can also contact the QuitLine on 13 78 48.

Late Effects Clinic
We care for and treat people who have ongoing health problems caused by cancer or cancer treatment.
Find out more