
More than 100 staff recently gathered at The Alfred to reunite with a patient whose care led to two world firsts and sparked a hospital partnership covering more than 3000 kilometres. This is how the occasion unfolded.
Former US Marine Travis Reyes holds two world records. He is the first person to ever undergo hyperbaric oxygen treatment while on ECMO life support, and his repatriation to the United States is the longest recorded ECMO retrieval flight in history.
Now discharged from hospital, Travis, along with his wife Jasmine and family, jumped on a video call to meet the Australians who saved his life.
For the clinicians, support and admin teams gathering at The Alfred and online, it was the first time they’d properly met.

“First of all I want to thank you for your service,” Travis said to the crowd.
“I literally owe you guys my life.
“It was weird going out of hospital and transitioning from military life back to normal civilian life.
“We’ve just been healing, we’re still healing; and we’re looking forward to the future and what’s next for us.”
*Image: Staff gather at The Alfred gather to meet Travis Reyes for the first time since he was in their care

In 2023, Travis was critically injured in a V22 Osprey crash during a military training exercise on Melville Island in the Northern Territory.
Emergency Physician at The Alfred Dr David McCreary happened to be working as part of the rescue retrieval team that was sent to the crash site.
“One of the clearest images I still have is arriving to find you surrounded by your fellow marines,” David recalled at the reunion.
"They had just pulled you out of the crash, and they were keeping you shaded with the shirts off their backs.
*Image: Travis Reyes and wife Jasmine Policarpio join the reunion via video call
“It seemed to capture the whole response. There was no ego, there was no noise. It was just people doing whatever they could for the person in front of them.”
Travis sustained a litany of life-threatening injuries from the crash, most critically in his chest and abdomen.
David performed a lifesaving thoracostomy, which helped to stabilise Travis until his arrival at Royal Darwin Hospital.
Nursing Director of Trauma Services at Royal Darwin Hospital Jenny Santhosh joined the reunion via videocall, alongside others in Travis’ Top End care and retrieval team.
“From the time you arrived at Royal Darwin Hospital, our teams worked with urgency and precision.” Jenny said.
“You moved swiftly through our emergency room, where it became clear you required lifesaving damage control surgery.
“You were then transferred to intensive care, but your condition continued to challenge every boundary of care,” Jenny said.
"The team determined the only remaining option to save your life was ECMO.”
*Image: Emergency physician Dr David McCreary spoke on behalf of Travis' emergency retrieval teams
At the time, Royal Darwin Hospital did not have an established ECMO Service, so the decision was made to transfer Travis to The Alfred in Melbourne, more than 3000 kilometres away.

Senior Intensive Care Specialist and the Clinical Lead of The Alfred ECMO Service Dr Arne Diehl was one of four specialists who assisted with Travis’ transfer in conjunction with aeromedical patient transfer service CareFlight.
“When we met you, you were very sick,” Arne said to Travis at the reunion.
“Your oxygen level was low, one lung was taken out and the other was bruised.
“It was an easy decision to put you onto the ECMO machine.”
The four of them took turns looking after Travis during the overnight flight to Melbourne.
*Image: Senior Intensive Care Specialist Dr Arne Diehl spoke on behalf of the ECMO retrieval team who oversaw his transfer from Darwin to The Alfred




On arrival, Travis was met by an extensive multidisciplinary team, led by The Alfred’s Deputy Director of Trauma Services A/Prof Joseph Mathew and Deputy Director of ICU Operations Dr Judit Orosz. Both were acting as department directors at the time.

Cardiothoracic surgeon Dr Julian Gooi, plastic surgeon A/Prof Scott Ferris and Infectious Diseases specialist Dr Andrew Fuller were also on hand to lend their skills, expertise and counsel

“The Darwin team did a wonderful job of saving your life by acting fast to remove your lung,” Julian said.
“When you came to The Alfred, you began to develop leaks in the area where your lung had been removed which was going to cause major problems.”
The team worked to stabilise Travis via multiple surgeries over the coming days.
ICU Trauma Clinical Nurse Consultant Kate Gibbon was among the nursing team that cared for Travis and his family during his stay.
“What stands out so clearly in all of our memories is the overwhelming pride and love that surrounds you,” Kate said to Travis.
“Through your friends and family, we came to know how remarkable a person you are.”

“They all were always there, holding your hand, stroking your head, letting you know that they were there, you were safe, and that you were always, always truly loved.
“Your family were always so appreciative of every little thing, be it washing your hair, giving you a shave or putting lip balm on your lips.”

Travis’ family were also supported by Eli Dannaoui and his family, who own and run Cafe Alfretti at The Alfred.
“During their time in Melbourne, Travis's family became a part of our world,” Eli said.
“They were here every day, holding a vigil, holding each other up, holding onto hope. And somewhere along the way, the team here at Cafe Alfretti took them in as one of their own.”
*Image: (From left) Jude and Eli Dannaoui
.mp4.00_02_48_14.Still001.jpg)
In the ICU, Travis was turning the corner.
“Initially you improved from day to day, up until day nine,” Joseph recounted at the reunion.
“But that changed when we noticed a little pimple on the right side of your face that had an abscess underneath.”
Biopsies showed that Travis had contracted fungal infections, likely from the mud, dirt and sticks at the crash site on Melville Island.
*Image: Travis' parents Karyn and Joe Reyes joined the reunion via video call

“There were two of them that are normally fatal, and that we normally only see in people who are immunosuppressed,” Andrew explained.
“One was called mucor and the other was fusarium, which is even nastier than mucor.”
The infections invaded blood vessels in Travis’ face, causing necrosis. The multidisciplinary team worked with A/Prof Scott Ferris who worked to debride – or cut away - the infected areas to stop the spread of infection.
Despite multiple surgeries, the infections spread further down Travis’ face and had almost reached his carotid artery; the two major blood vessels that supply blood to the brain, neck and face.
Further surgical treatment would have involved taking extreme measures: tying off the carotid artery, which would result in paralysis down one side of the body, in addition to the debridement of Travis’ entire face and the removal of his infected cheek and jaw bones. He would then need to wait another two years to receive a facial transplant.
“The overwhelming response from Jasmine and your parents was that this option would not reflect your values, and that you would want to have a functional life going forward,” Joseph recounted.
“And that’s when we started to consider experimental therapies.”



One of the options, which had been raised earlier during Travis’ time at The Alfred, was Hyperbaric Oxygen Therapy.
The Alfred’s Head of Hyperbaric Dr Bridget Devaney had seen firsthand the positive effect it had on the handful of patients she treated with mucormycosis, the same infection that Travis was suffering from.
“When you first came to us, it wasn’t an option,” Bridget said at the reunion.
“You were on ECMO, and no one in the world on ECMO had ever received hyperbaric oxygen therapy before.”
But as Travis’ condition deteriorated and the range of treatment options continued to narrow, what might have been deemed too risky a week or so earlier began to look like his best option.
“The possibility that we might cause you harm by trying this was previously completely unacceptable,” Bridget said to Travis.
“It looked different in the light of a last-ditch effort to save your life.


For some years leading up to this moment, The Alfred’s hyperbaric engineers had been developing a modified ECMO machine that could function safely in the hyperbaric chamber.
“We knew it was physically safe in the chamber,” Bridget said.
“There was no fire risk, no risk to staff.
“We knew that it functioned normally with saline in the circuit, but we didn’t know how it would behave at pressure with a patient attached and blood in the circuit.”
Joseph, Judit and Bridget sat down with Jasmine and Travis’ family to talk them through the risks and possibilities of such an approach.
“I want to acknowledge the decision that Jasmine and your parents made on your behalf that day,” Bridget said to Travis.
“They believed that even if you didn't make it, you would have wanted us to try.
“It was hoped that by doing so, we might one day be able to help someone else.
“I also want you to know what a rock Jasmine was in those moments.
“She handled the entire situation with grace, poise and calm; she took in all the information and asked excellent questions.
“She told me that you were 'one in a million’ – a fact that I think has since been scientifically proven.”
With the blessing of Travis’ family, things moved quickly.
The Alfred’s executive team – led by Deputy Chief Executive and Chief Operating Officer Simone Alexander and Deputy Chief Operating Officer Josh Stuart – worked with clinicians and governing bodies through the night to ensure Travis’ treatment could go ahead as soon as possible.
.jpg)
“There is a wonderful partnership between senior clinicians and executive at The Alfred, and your case, Travis, is one of the finest examples,” Josh said at the reunion.
“Briefing and approval meetings, out of session committee approvals and clinical and logistical coordination kicked in immediately and moved at pace.
“When there is a need, we also have a strong will.”
Just 32 hours later, Travis Reyes became the first person in the world to undergo hyperbaric oxygen therapy while on ECMO.
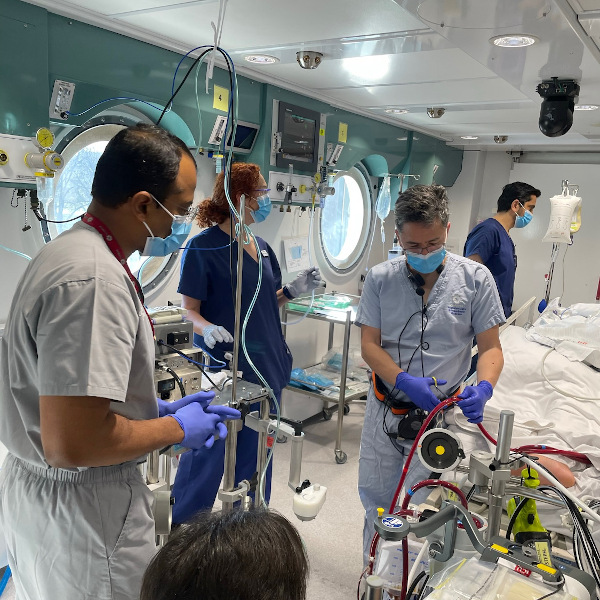

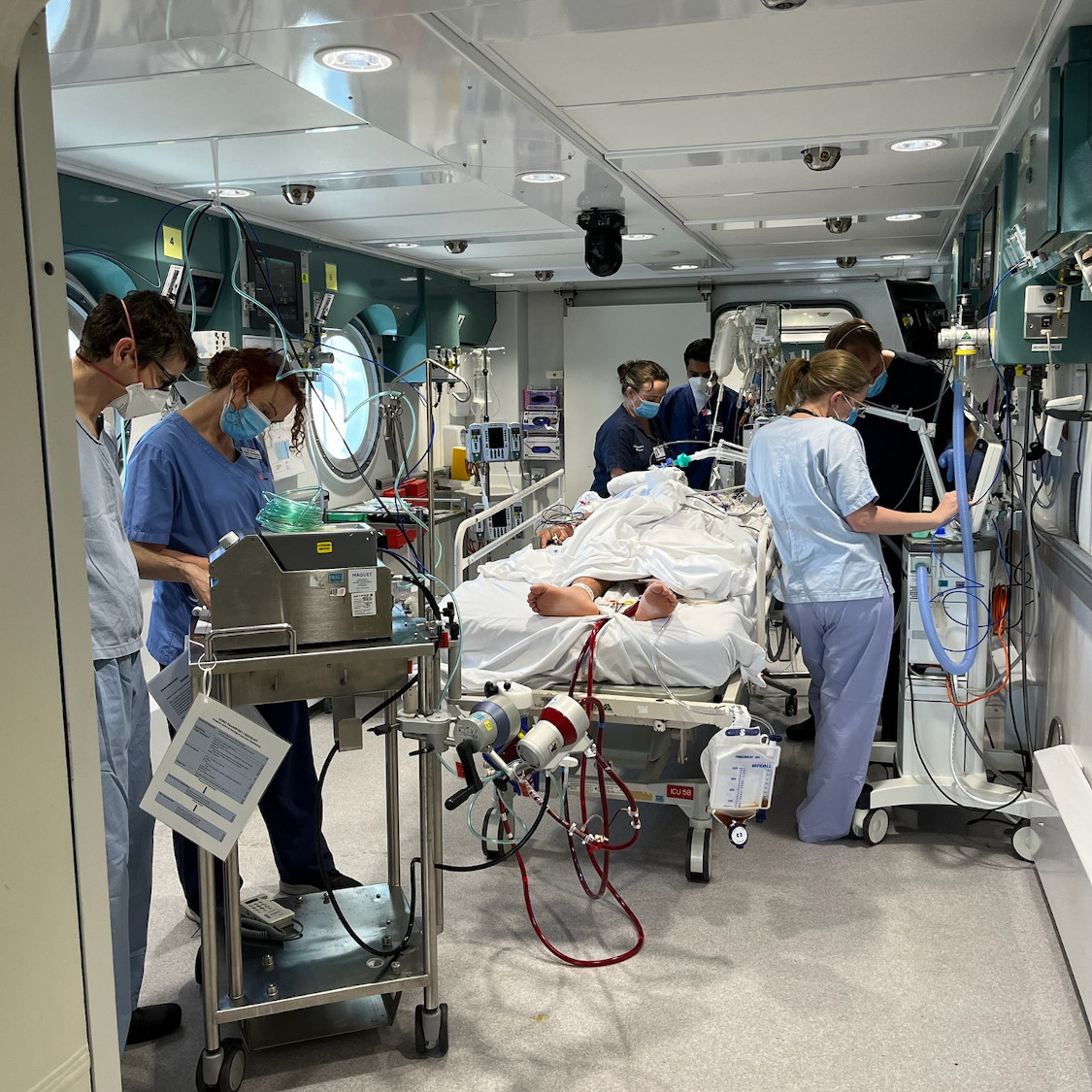
After a successful first session, Travis went on to have 13 hyperbaric treatments, lasting 95 minutes each.
“By the tenth treatment, the fungus on your face had cleared up, and the fungal infection in your blood had improved,” Joseph said.
“You were also significantly less reliant on the drugs being used to support your blood pressure.
“When we lightened your sedation, you were able to obey commands and move all four limbs.
“And most importantly, you were relatively stable.”
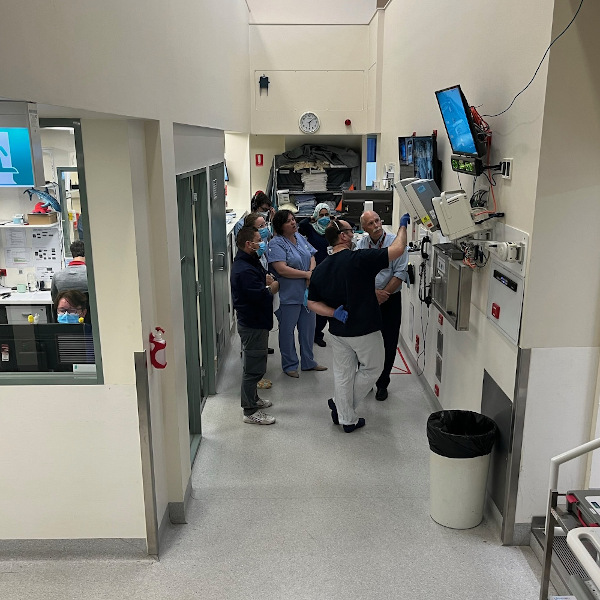

Throughout this time, briefings between Travis’ Australian and US medical teams were happening daily. His newly stable condition presented a window of opportunity to bring him home to continue his recovery and rehabilitation.
That’s when The Alfred initiated another world first: the longest ever ECMO retrieval at just over 14,000 kilometres from Melbourne to Texas.




The Alfred’s Clinical Service Director for the ICU and Hyperbaric Services Tania Birthisel worked closely with Travis’ medical team to ensure his safe transfer from The Alfred to Melbourne Airport, where Travis would be put into the care of his US Military medical team.
“I still remember waving to you as the door of the C-17 Globemaster was closing as you were about to embark on that journey to bring your husband and son home,” Tania said at the reunion.
"In that moment, I had a feeling our paths would cross again and here we are.
“It's truly an honour to be able to say hello again.”
*Image: Clinical Service Director for The Alfred ICU and Hyperbaric Services Tania Birthisel spoke on behalf of Travis' ICU care teams

The plane took off in the early hours of the morning. Back at The Alfred, ICU staff followed an online flight radar to follow the journey Travis and his family were making to Texas.
As the reunion was coming to a close, Travis said he was at a loss for words.
“There was a lot that I didn’t know about until tonight,” Travis said.
“Words can’t explain how grateful I am for everybody.”

Bayside Health Alfred Chief Executive Simone Alexander said Travis’ case has left “an indelible legacy on our healthcare system”.
“On behalf of all of us here at The Alfred, we want to thank you, Travis and Jasmine, for this opportunity to reconnect,” Simone said.
"It's hard to adequately describe the impact you've had on all of us, both personally and professionally, but you've heard some of it today.
"You were the first patient to undergo hyperbaric therapy while on ECMO.
“You were the centrepiece to the longest ECMO retrieval in world history.
“Your time with us led to the establishment of a partnership between the Alfred ICU and Royal Darwin Hospital, which now provides ECMO training and intensive courses, as well as an ECMO retrieval program between our two hospitals.
“For every patient who has come after you, we can now do things we didn't think possible before.
“We are so happy to see you again, to see you surrounded by your loving family, and to see you getting back to doing the things that you love.”
